When you have a tooth extracted, your dentist may warn you about dry socket and tell you how to prevent this complication. You should definitely follow that advice, because dry socket pain is excruciating. But what is dry socket, exactly, and what symptoms should you look out for?
After your tooth is removed, a blood clot forms in the empty socket to protect the nerves and bone below while your mouth heals. Dry socket occurs if that blood clot becomes dislodged, and the pain comes from the nerves being exposed. Fortunately there are several precautions you can take to reduce the chances of this happening, which we will explain later on.
This article will also answer common questions such as:
- What does dry socket look like?
- How common is it?
- Will dry socket heal on its own?
- Can I get treatment on the NHS?
- What is the average healing time?
- When can I stop worrying about dry socket after an extraction?
We hope this helps you understand more about this oral health condition and – hopefully – avoid developing it yourself.
What is dry socket?
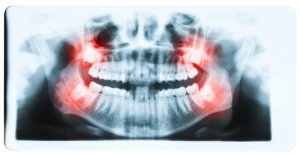
Dry socket, or alveolar osteitis, occurs when the blood clot present at the site of a tooth extraction dissolves or becomes dislodged. This blood clot is usually responsible for protecting the nerves and bone tissue present at the extraction site during the entire healing process. Without this blood clot, the sensitive area beneath is exposed, making the socket vulnerable to further trauma and bacteria.
How common is it?
Fortunately, only a small number of people who have a tooth extraction develop problems like alveolar osteitis. While more research is needed, most dental experts believe that less than 1 to 5 percent of people develop dry socket after tooth removal.
There are some factors that can increase your risk of experiencing dry socket::
- You are more likely to suffer from a dry tooth socket during the first seven days following removal.
- The problem hits teeth in the lower jaw more than teeth in the upper jaw.
- Molar extractions are more at risk of developing dry socket symptoms, especially when the dentist or oral surgeon is dealing with a surgical wisdom tooth extraction.
What causes dry socket?
The main cause of dry socket is a partial or a complete loss of a blood clot in the tooth socket following extraction. This blood clot forms in order to protect the exposed socket and the jawbone present beneath the teeth. If this blood clot gets lost or does not form at all, the underlying jawbone is exposed and healing is delayed.

Now let’s have a look at some of the other factors that can contribute to dry socket complications:
- Bacteria: Any pre-existing infection of the oral cavity prior to tooth extraction (e.g., gum disease) may cause an improper formation of the blood clot. Even if the blood clot is somehow formed, the oral bacteria present in the mouth may cause it to break down.
- Chemicals: Nicotine is one of the most common chemicals known to have a severe negative effect on oral health. Abundantly present in cigarettes, this chemical can reduce the blood supply in the oral cavity which hinders the formation of the blood clot at the site of tooth extraction.
- Abrupt movements: Performing certain activities such as aggressive rinsing, sucking through a straw, and forceful spitting after a recent extraction can dislodge the blood clot and lead to alveolar osteitis.
- Biological factors: Certain factors, like having a dense jawbone, hormonal imbalances, and a poor blood supply, can hinder the formation of the blood clot. This drastically increases the chances of acquiring a dry socket following tooth removal.
Interestingly, the reason for the tooth extraction can also affect your chances of developing dry socket. Some research suggests that extractions which are a result of poor oral health (e.g., tooth decay or periodontal disease) are more likely to result in this painful condition.
Here are some other things which may increase the chances of getting alveolar osteitis:
- Undergoing a difficult tooth extraction
- Taking oral contraceptives or birth control pills which can also interfere with the healing process
- Using tobacco or nicotine products within 48 hours of surgery
- Not taking care of your oral health after extraction of the tooth
- Having a history of dry socket
- Frequent spitting after extraction of the tooth, which dislodges the clot
What are the main dry socket symptoms?
If you’ve just had a tooth out, you’ll want to be aware of the symptoms of dry socket as well as some prevention measures. You might also want to know what dry socket looks like.
We’ll spare you from any dry socket pictures, although you can view some images in this video if you really want to! If you look at a dry socket tooth you will see that the tissue inside looks dry rather than moist, and instead of a dark red blood clot, white bone might be visible. If the extraction site is at the back of your mouth, especially from a wisdom tooth, it might be difficult to check visually (and you should be careful not to touch it as this may cause further infection).

Even if you can’t see the socket clearly, you’ll probably know about it from the pain. It’s normal to experience some pain for a day or two following tooth extraction. However, a common dry socket symptom is a persistent throbbing or stabbing pain that begins or worsens a few days following tooth removal. The pain normally radiates to surrounding areas of the face. Drinking cold beverages, eating, or merely breathing may cause extreme pain and discomfort in the mouth.
Some other dry socket symptoms include:
- Bad breath
- An unpleasant taste in the mouth
- Pain in the ears, eyes, jaw or neck
- A headache
If you are experiencing any of these signs of dry socket, especially if you can see that there is no blood clot, you should contact your dentist for advice. They will probably ask you to book an urgent appointment for a full assessment.
Diagnosis and cost
The presence of pain and other symptoms of dry socket is usually enough for the dentist or oral surgeon to make a diagnosis. The dentist will also examine your oral cavity to check if there is a blood clot in your tooth socket or if there is an exposed bone.
You may also be required to go through certain tests such as x-rays in order to rule out other conditions like bone infections or the presence of small bone fragments embedded in the wound following tooth removal.
If your tooth extraction was done by an NHS dentist, the dry socket treatment should be provided on the NHS for no extra charge, provided you return to the same dentist.
A private dentist may or may not charge extra for follow-up treatment after an extraction. It may depend on whether you need an x-ray and what treatment is required. You might be able to get treatment for dry socket on the NHS having had the tooth extracted privately, in which case standard NHS dental charges will apply.
Dry socket treatment
Wondering how to treat dry socket? The primary aim of the treatment is to decrease the intensity of symptoms, especially dry socket pain, and promote healing of the wound.
Dry socket treatment usually involves the following steps:
- Flush out the socket: Your dentist will start by flushing out the socket to get rid of food particles, dead tissue, or anything else that has made its way into the socket. This helps provide dry socket pain relief and allows the tissue to heal better.
- Apply a medicated dressing: The next step is to pack the socket with a medicated dry socket paste or gel and then cover it with gauze. This helps fight bacteria and promote healing. Dentists may also use a kind of dry socket packing that dissolves by itself after 3-5 days.
- Pain medication: Your dentist may prescribe some medication for your dry socket pain, or advise you to take over-the-counter painkillers.
- Self-care: Your dentist will advise you on how to treat the dry socket yourself at home. You may need to change the dressings and flush the wound out using saltwater or medicated mouth rinse. It’s important to follow your dentist’s instructions to reduce your dry socket healing time.
How long does dry socket last?
Once the treatment begins, you will soon notice some pain relief. The pain, along with other symptoms, will continue to improve over the next few days. After seven days the site should be completely healed. However, it is important to keep in touch with your dentist for regular dressing changes and oral care.
Will dry socket heal on its own?
You might be tempted to stay home and just take painkillers until you feel better. Sticking to dry socket treatment at home might work in some cases, but we recommend speaking to your dentist first.
Why? The blood clot not only protects you from pain; it also stops bacteria and food from getting into the socket and causing infection. So, without a blood clot, the chance of infection and further complications increases. It will also take longer for the dry socket tooth to heal if you don’t get it treated.
How to prevent dry socket: Surgical care
Are you about to undergo tooth removal? If so, it’s important to be informed about dry socket prevention. The following are some of the things you and your dentist can do before and after the surgical procedure.
What can you do before surgery?
The following measures can be taken before surgery in order to prevent a dry socket.
- Go to a dentist who has experience in dental extractions.
- If you are a smoker, try to avoid smoking a few days before the surgery as the use of tobacco products can increase the risk of dry socket.
- Let your dentist know if you are taking any over-the-counter or prescription medicines as they may interfere with the clotting of blood.
What can your dentist do?
Your dentist can take several steps to help your mouth properly heal following the surgery in order to prevent dry socket. This usually includes using certain medications such as:
- Antibacterial gels or mouthwashes both before and after surgery
- Antiseptic solutions applied to the wound
- Oral antibiotics, especially if you are immune-deficient
- Medicated dressings applied to the wound after surgery
After the surgical treatment, the dentist will instruct you about what to expect during the recovery process and how to take care of the wound. Following a proper plan for tooth extraction recovery can significantly promote healing and prevent complications.
How to prevent dry socket: Homecare
Is there a home remedy for dry socket? Can taking measures at home prevent this problem from developing in the first place?
Absolutely! There are some simple steps that you can take in order to reduce your chances of suffering from a dry socket. Remember, this condition most commonly occurs when some exterior force dissolves or dislodges the protective blood clot from the socket, so your aim should be to keep the clot in place until your mouth has completely healed post-surgery.
You should always follow your dentist’s advice to prevent dry socket after tooth extraction, but perhaps you don’t remember that clearly what they told you or you want some more tips for avoiding a dry tooth socket. In that case, here’s what you should do:
Rest and recuperate
After surgery, make sure to rest for the remainder of the day. Consider taking the following day off work (or scheduling your surgery for a Friday) so you have that extra day to recover. Your dentist will tell you how long to stay away from sports and other strenuous activities to prevent the blood clot from dislodging.
Manage the pain
To relieve pain and swelling from the extraction, you can alternate placing ice packs (wrapped in a tea towel) and warm compresses on your cheek. Of course, you should also take any pain medication you have been prescribed.
For some home remedies for dry socket pain, including clove oil, our tooth pain home remedies article is a good resource.
After an extraction, I recommend to my patients the following dry socket prevention tips:
- One of the main reasons people develop dry sockets following extractions is frequent spitting after the procedure to get rid of the taste of blood. I advise my patients to try to swallow their saliva including the blood, instead of spitting it out, as this disturbs the formation of the blood clot at the bottom of the socket.
- If the patient is a heavy smoker and absolutely must smoke within the first 48 hours after surgery, I advise them to put a gauze over the extraction site to cover and protect the socket and its blood clot.
- In case there is excessive bleeding following the extraction, patients should place a wet tea bag over the extraction site to both reduce the bleeding and protect the blood clot.
- I also recommend that patients eat pineapple or drink pineapple juice before any surgeries and after it because the bromelain in pineapple helps to reduce the inflammation, pain, swelling and bruising that could develop following any surgical procedures including extractions.
Dr. Joseph Salim, Sutton Place Dental Associates
Stay away from straws

When you use a straw to drink, the sucking action creates a vacuum in your mouth. This vacuum can pull the blood clot out of place, so you should completely avoid the use of straws for at least one week following dental extraction.
Also stay away from carbonated, caffeinated, hot, and alcoholic beverages for as long as advised by your dentist.
Eat soft food
For a day or two after surgery, stick to soft foods like smoothies, soups, mashed potato and yoghurt. Avoid very hot or cold food, and be careful about biting your cheek until the anaesthesia wears off.
Switch to semi-soft foods when you feel like you can easily tolerate them, but chew on the side of the mouth away from the extraction. Stay away from sticky, chewy and crunchy foods for at least a few more days to avoid damage to the site.
Adopt proper oral hygiene
Maintaining good oral hygiene is among the most important ways to prevent dry socket.
Ask your dentist about how to brush your teeth after surgery. In most cases, you will be advised to just gently rinse your mouth on the first day following surgery, and switch to gentle tooth brushing on the second day. You may also be asked to use an antibacterial mouthwash and gauze pads a few times a day.
When using a mouth rinse, be very careful not to swish it around too vigorously, especially for the first 24 hours. Instead, put some in your mouth and move your head around so it covers the extraction site.
Once you are past the first 24 hours, you can use warm salt water to rinse your mouth a few times a day following surgery. To make this rinse, mix 1/2 teaspoon of table salt in a small glass of warm water and mix until dissolved.
Say ‘no’ to tobacco
People who routinely use tobacco are at a greater risk of dry socket following dental extraction. One study found that this problem occurred in approximately 12% of individuals who smoked after an extraction. In comparison, only 4% of non-smokers who underwent dental treatment developed a dry socket.
Inhaling cigarette smoke after tooth removal can dislodge the blood clot for the same reasons as sucking a straw can. Furthermore, the chemicals present in tobacco products can also interfere with healing and may lead to the development of a secondary infection.
Hence, most dentists advise reducing your tobacco intake for at least a few days prior to dental surgery as well as in the days following it.

If you find you experience withdrawal symptoms, the following can significantly decrease your risk of acquiring a dry socket:
- Switch to a nicotine patch for the time being
- Wait for at least 48 hours post-surgery before resuming smoking after tooth extraction
- Ask about getting stitches on the surgical site
- Avoid chewing tobacco or nicotine gums
If you do want to resume using tobacco after the treatment, ask your dentist about when you can safely start. As a general rule of thumb, you must wait for at least 48 hours; however, this may vary from person to person.
Conclusion
What is dry socket? It’s an extremely painful condition that can happen following a tooth extraction if the blood clot doesn’t form properly or is dislodged. However, a simple dry socket treatment with your dentist should ease the pain immediately and the total dry socket healing time is around seven days.
There are also plenty of ways to prevent dry socket even before your extraction takes place. Follow your dentist’s advice and take some extra precautions using the tips in this article. If you do notice any dry socket symptoms developing in the days after your treatment, speak to your dentist straight away.
For a quick recap, watch this dental nurse explain what dry socket is and how it’s treated:
FAQs
Why is the blood clot needed for the healing process?
The clot serves as a protective barrier against bacteria and other types of irritants that may lead to infection. It also plays a crucial role in the growth of new tissue and bone at the extraction site.
What does a dry socket look like?
If you can see inside the socket, you’ll notice that there is no dark, red blood clot. Instead, the tissue inside looks dry and the white bone may be visible.
How long does dry socket take to heal?
Dry socket normally occurs within 3 to 5 days following the extraction. The usual dry socket healing time is 7 days, of which the first 3 days are the most painful. If the condition persists beyond this time, further investigation is warranted.
How long should dry socket packing stay in?
If your dentist uses a gel or foam packing which is designed to dissolve by itself, it will stay in for three to five days before starting to liquefy and disappear. This should be adequate time for the tissue below to being healing.
What questions can my dentist ask me?
Your dentist may ask one or more of the following questions before a treatment for dry socket:
- When did the pain begin?
- When did it get severe?
- Does the pain occur spontaneously or is it triggered by any activity such as touching the affected area?
- Where is the pain located? Does it radiate?
- On a scale of 1 to 10, how would you rate your dry socket pain level?
- Have you already taken any painkillers? If yes, what is the dosage and frequency of these medications?
- Does using painkillers reduce the pain?
- Are there any other symptoms not related to this pain?
What complications can develop from dry socket?
The most common complication of dry socket is delayed healing. Infections may also occur; however, these might not be strictly associated with alveolar osteitis. If you develop any sign of infection, contact the dentist immediately. The most common symptoms include:
- Fever
- Redness and swelling
- Discharge from the extraction site
Oral Health Dent Management: Prevalence and association of dry socket in oral health and dental management. Consulted 2nd April 2020.
International Journal of Dentistry: Alveolar osteitis: a comprehensive review of concepts and controversies. Consulted 10th Feburary 2020.
The Open Dentistry Journal: Dry socket: frequency, clinical picture, and risk factors in a palestinian dental teaching center. Consulted 10 Feburary, 2020.
Journal of Clinical and Diagnostic Research (JCDR): Systemic review of dry socket: aetiology, treatment, and prevention. Consulted 10 Feburary, 2020.




