Facing a root canal treatment and feeling anxious? You’re not alone. This essential dental procedure, while daunting, is crucial for saving a decaying tooth and preventing future complications.
Our comprehensive guide covers everything you need to know about root canal treatments in the UK, including:
- What is root canal treatment?
- What is the procedure in the UK?
- How much is a root canal? NHS and private costs
- Does a root canal hurt?
Dive into our article for insights on root canal treatment cost in the UK, infection symptoms, recovery tips, pain management strategies, crowning processes and costs and insurance coverage.
Save the trip to your NHS dentist and speak to a certified dentist right now online. Visit JustAnswer to chat online with a qualified dentist and find out all the information you need – without having to take time out for a dental appointment.
Their dentists are based in the US and are available 24/7 to help you out!
What is root canal treatment?
The root canal system is located in the roots of each of your teeth. A tooth root infection, if left untreated, can cause irreparable damage to the tooth and even spread to other parts of the body.
The root canal procedure, an endodontic treatment sometimes referred to as a ‘root filling’ or just a ‘root canal’, involves drilling right inside the tooth to remove decay and infection deep down in the roots.
This work may be performed by a general dentist or by an endodontist, who specialises in treating the inside of a tooth.
Once the root is treated, the root and tooth are filled to help preserve the remaining tooth. Teeth that have undergone root treatment are more fragile than healthy teeth. Your dentist may therefore recommend fitting a dental crown to help prevent further damage.
The tooth structure
Before we get into the details of what root canal work involves, it’s helpful to understand a bit about the structure of a tooth.
The crown is the part which sticks up above the gum line. The section level with the gum line is called the neck, and the part below the gum is the root. The tooth root can be twice as long as the crown.
Get a free quote for dental treatment abroadA root may split into two canals, meaning that teeth usually have up to four root canals each. In some rare cases, six or seven roots have been found in one tooth!
The hard white coating outside the tooth crown is called enamel. This is the part you need to protect by brushing and flossing daily. A build-up of bacteria on the teeth resulting from poor oral hygiene can lead to dental caries (tooth decay).
If tooth decay erodes even a small amount of enamel, it leaves the rest of the tooth susceptible to infection. Once bacteria starts eating away at the soft dental pulp inside the tooth it can quickly spread down the tooth root(s) through the root canal system. From here it can reach the surrounding bone and gum tissue.
Untreated root canal infections are likely to lead to an oral abscess.
When do I need root canal treatment?
An infected root canal usually develops quite slowly, from untreated tooth decay which has led to pulpitis. When a tooth has undergone multiple restorative procedures, or when a crown or filling is loose or faulty, there is a higher chance of root infection. In some cases, the infection can develop more quickly. For example, if you experience facial trauma or get a cracked or broken tooth.
If you have regular dental checkups, your dentist will be able to identify and treat any tooth decay before it penetrates the root system. However, if you haven’t been to the dentist for a while, you may find the infection has already spread and you need root canal therapy to save the tooth.
Symptoms that indicate that tooth pulp has become infected may include sensitivity to hot/cold or sweets, pain, swelling, pain to biting or pressure, and a bad taste in the mouth. However, sometimes no symptoms are apparent and you may be unaware of any problem until a checkup. (This is just one of the many reasons to make and keep your 6-month appointments.) These dental checkups and cleanings can prevent small problems from becoming big issues.
Keep in mind that not all types of tooth pain mean you need a root canal. We suggest that you make an appointment with your dentist if you notice anything out of the ordinary with your teeth or mouth.
Dr. Robert Berry, Mountain Aire Dentistry
Root canal infection symptoms
Initial signs that you might need root canal work include:
- Your tooth is painful or sensitive to hot and cold food and drink
- It hurts to bite down
- One of your teeth is loose
If you ignore these root canal symptoms, you may find they disappear over time. This isn’t because the infection has healed itself – it means it has destroyed the nerves contained in the dental pulp so you can no longer feel it.
Eventually, you’ll notice these symptoms returning, possibly along with the following signs that the tooth has died and the infection has spread much further:
- Swollen gums around the infected tooth
- Swelling in your face
- Pus oozing from your tooth or gum
- Discolouration of the tooth
Going to the dentist as soon as you experience any kind of tooth pain should help prevent the infection from spreading to this more serious stage. The tooth root won’t heal itself, and the longer you leave it, the less chance there is of root canal treatment being successful.
We don’t recommend relying on antibiotics to clear a root canal infection without any other dental treatment. Although you may be given antibiotics as part of your treatment, medicine alone won’t be enough to return your tooth to a healthy state.
If your root canal pain comes on suddenly and over-the-counter painkillers have no effect, you should book an emergency dentist appointment. They may not perform an emergency root canal immediately but will give you stronger pain relief until you can receive the treatment you need.
Do I need root canal treatment or a complete tooth extraction?
The main priority of your dentist should be to preserve your natural teeth for as long as possible. However, if the bacterial infection has spread through most of the tooth, and the remaining structure is not enough to support a filling or crown, extraction may be the only option.
When a tooth is extracted, it can affect how you eat and put extra strain on the surrounding teeth. Over time the jaw bone at the extraction site can recede, causing changes to your facial appearance.
You will be able to save money when opting for an extraction rather than a root canal, however, you’ll also have to replace the missing tooth, which will cost more in the long run.
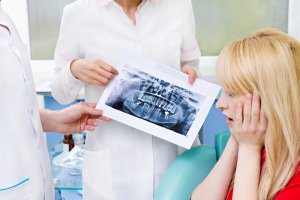
Your dentist or root canal specialist will usually begin by taking x-rays of the affected area to determine the extent of the infected root canal. From these images they will be able to see how many canals the affected tooth has, where they are positioned, and how many of them require treatment.
They can then plan your procedure and let you know what to expect.
Note that if you have an infected wisdom tooth, there are certain situations where your dentist may opt to extract it rather than perform a root filling. If the tooth hasn’t fully erupted, for example, or is in a position that’s difficult to clean, your dentist may recommend extraction.
How long does root canal treatment take?
It’s possible to complete a simple root canal treatment in 30 to 60 minutes. More complex procedures, or those involving multiple teeth, will take longer. Multiple visits may be needed to complete your treatment course in this case.
Root canal treatment time depends on several factors:
- Which tooth is being treated
- The number of roots and canals, and their shape
- The amount of infected tissue
- Type of tools that your dentist uses
We recommend discussing the procedure with your dentist ahead of time so you know what to expect. Luckily, modern advances in dentistry mean that it is getting easier to complete the process quickly and with minimal discomfort.
How long does root canal treatment last?
Endodontics is a common dental practice with a relatively high success rate. Around 85% of treatments last for at least 8-10 years – if the patient maintains good oral hygiene. Many go on to last a lifetime. Giving up smoking (if you currently smoke) will help prolong the effectiveness of any dental work while improving the overall state of your teeth.
If you experience tooth pain years after a root canal, it may be possible to perform a root canal re-treatment and preserve the tooth for even longer.
One downside of root canal treatment is the tooth may darken over time. However, with modern endodontic techniques, this is becoming less common. If you do experience discolouration after root therapy, especially with a front tooth, you may consider getting it chemically whitened.
Root canal treatment procedure
There are six main root canal treatment steps needed to restore a deeply infected tooth.
Front tooth root canals tend to be more straightforward since they are easier to access and the canals are generally straighter and wider. This means that a root canal on a front tooth is usually quicker to complete than on a tooth at the back of the mouth. However, your dentist can’t know for certain how complex the treatment will be until they access your tooth roots.
We have already mentioned that before any procedure is done, your dentist will first do an x-ray to determine the course of treatment.
The exact root canal treatment procedure will vary slightly from one clinic to another, but here is a basic outline of the steps involved:
Step 1: Preparation
In preparation for a root canal treatment, your dentist or endodontist will administer a local anaesthetic. This numbs the area being treated so you shouldn’t feel any pain.
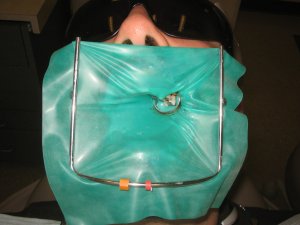
It’s good practice for dentists to fit a waterproof dental dam (cofferdam) while doing root canal work. This rubber sheet fits around a single tooth to isolate it from the rest of your mouth.
The dental dam serves three main purposes:
- It protects the inside of the tooth from bacteria in your saliva
- Allows you to swallow normally during treatment
- If the dentist accidentally drops a tool or some debris falls into your mouth, there is no risk of you swallowing it and choking
It’s possible to perform this work without a dental dam, but according to a study done by PubMed, a rubber dam “provides a significantly higher success rate of root canal-treated teeth”.
Step 2: Opening the tooth
Using a drill, the dentist will make a hole in the top of your tooth (or at the back of a front tooth) through which he can access the pulp chamber and root system. Tiny little files or a mechanical rotary tool help clear away the damaged and dead pulp and nerve tissue from inside the tooth and roots.
Root canals are very thin and are often curved, so it can take some time for the dentist to locate all of the canals and ensure all traces of infected material are removed. They use special microscopes and bright lighting to help them see right inside the tooth.
If you have a root canal abscess at the end of your tooth root, it will be drained at this point.
Step 3: Cleaning
Next, the inside of the tooth is cleaned thoroughly using water and an antibacterial solution. Your dentist uses a syringe to squirt the cleaning solution into your tooth, then it is sucked back out. This is repeated several times throughout the process to ensure the area is completely sterile.
Step 5: Root shaping
The narrow and irregular shape of root canals makes them difficult to fill properly. Therefore, one of the most important root canal treatment steps is to enlarge and shape each canal in the tooth. There are several reasons why this is necessary:
- It ensures the full removal of necrotic pulpal tissue and bacteria from the canal space
- It creates optimum space for the root-cleaning process and root-filling
- The resulting smooth tooth structure is preferable for long-term preservation
If your dentist uses traditional hand files, this part of the procedure can be very lengthy and require multiple visits. Modern mechanical rotary tools make it faster and more effective.
Using a mechanical rotary tool has several benefits over traditional hand files:
- More accurate cleaning and shaping of the canal
- Easier and more accurate filling
- Significant reduction in post-operative sensitivity
- Less discomfort and dental chair time required to finish treatment
- Less risk of damage to the healthy tooth structure
Because of the shorter treatment time and more comfortable recovery, you may wish to select an endodontist near you who will use a rotary tool rather than hand files for your treatment.
– Dr Eyad Tariq
Step 6: Root filling
If your treatment is too complex to complete in one visit, your dentist will fill the roots with some medication to kill any remaining bacteria. He will then apply a temporary filling to protect the tooth between visits. This temporary filling is removed when you return to complete your treatment.
Once all the canals have been cleaned and widened, it’s time to permanently fill them. This is often done with a thermoplastic material which, when heated, softens to fit the exact shape of the chamber. Dentists insert multiple thin cones into the canal and then compress them under heat to ensure complete filling.
It’s important that the root canal filling completely fills the space inside the tooth. Otherwise, the filling could fall out and it’s more likely to become re-infected.
Once the roots are filled, the remaining space in the tooth is filled and restored just like a regular tooth filling. This provides an extra seal to protect the roots from any more bacteria.
Step 7: Crowning (optional)
Because your tooth is more fragile following endodontic treatment, the dentist may recommend that you have root canal treatment together with an optional dental crown. A crown (also called a ‘cap’) is a protective covering made from porcelain or metal. It covers the entire tooth and should prevent a cracked tooth after root canal work.
To fit a crown, your dentist first has to shave some of the enamel off the outside of your tooth. They use strong dental glue to keep it in place. Once fixed in place it should feel and function just like a natural tooth. The root canal and crown cost will be higher than that of just a root canal, however, your dentist will recommend what’s best for your tooth.
Your dentist may wait a few weeks before crowning your tooth, just to be certain that the process was successful and there are no signs of infection after the root canal filling.
The video below gives a quick summary of the whole procedure:
Root canal treatment cost in the UK
A root canal treatment cost ranges from £100 to £700 in the UK with a private dentist. As a general rule, the more complex the procedure, the longer it will take and the more it will cost. You can also get an NHS root canal treatment for a lower price if you are registered with an NHS dentist.
How much is a root canal on the NHS?
If you get a root canal on the NHS, the Band 2 charge applies. For 2023/24 this stands at:
- £70.70 in England
- £47.00 in Wales
- Variable prices in Scotland and Northern Ireland
This flat fee applies regardless of how many visits you need or how many teeth are treated (provided it all relates to the same course of treatment). So, the cost of NHS root canal treatment is relatively inexpensive.
The root canal and crown cost on the NHS is the Band 3 charge of £282.80 (England) or £203.00 (Wales).
However, not everyone can find an NHS dentist accepting new patients. In this case, you will need to see a private dentist, resulting in the root canal price being significantly higher.
How much is root canal treatment privately?
Root canal prices with a private dentist in the UK range from £100 – £350 for front teeth and £300 – £700 for back teeth.
The exact cost of a root filling with a private dentist will depend on:
- Your dentist’s location and private rates
- The extent and complexity of the damage
- Tooth size (specifically, the number of roots and canals)
- Tooth position (those at the back tend to cost more)
Dentists and root canal specialists will most likely not be able to give you a fixed root canal price until they have examined your mouth and taken X-rays to assess the condition of your teeth.
You may still be able to get an idea of root canal costs by enquiring with different clinics though, and it’s worth doing this as prices can vary quite substantially from one to another.
What’s the difference between NHS and private root canal treatment?
Both NHS and private dentists will work to remove any infected tissue from your tooth and repair it to a functional state. The result should, in theory, be the same.
However, some may argue that a private dentist can dedicate more time to you and carry out the procedure with more care and attention since they are not under the same pressure as NHS dentists.
Insurance for dental treatment
Many dental insurance plans cover endodontic work to some extent. Feel free to ask your dental insurance provider what percentage of root canal treatments it will cover, and how to schedule your appointment.
It can be beneficial to have dental insurance if you have oral health problems and will need a lot of dental work in the future. Our article on dental insurance in the UK has more information on how to choose a policy to suit your needs.
Is root canal treatment painful?
Many patients fear root canal treatment pain and end up postponing their appointments. Fortunately, the anaesthetic technology used by dentists means that the procedure can be performed with minimal discomfort. The procedure should feel similar to having a regular filling, except it will take longer and you may feel stiff afterwards since you have held your jaw open so long.

For patients experiencing significant root canal pain before treatment, getting endodontic therapy provides considerable relief.
Your dentist will administer anaesthetic before starting any work and may “top it up” during longer treatments. As a general tip, you can tell your dentist you will raise your hand if you start to feel uncomfortable at any point.
Particularly nervous patients have the option of IV sedatives while the work is done. Although you won’t be completely unconscious as you would be with a general anaesthetic, you will feel deeply relaxed.
Pain management after root canal treatment
Root canal recovery shouldn’t be painful, but your restored tooth may be swollen or sensitive for a few days. During this time you can take ibuprofen or paracetamol to ease any discomfort.
You may find it more comfortable only to eat soft foods until your mouth is back to normal, especially if you feel pain when biting on the treated tooth.
Yes, patients may experience a little discomfort or pain after root canal treatment, once the anaesthesia wears off. This is a side-effect of the root canal cleaning and preparation procedure.
This can last for 1-2 days, but over-the-counter painkillers should relieve any pain.
If you experience continued throbbing pain after taking painkillers or develop severe pain a few days after your root canal treatment, you should immediately contact your dentist. This is a sign of a failed root canal procedure and you may need extra dental care.
– Dr Eyad Tariq
Possible complications and problems during treatment
Despite the relatively high success rate of endodontic treatment, some patients do experience problems. Root canal complications can occur anywhere from a few days to a few years after the initial treatment.
A failed root canal can be the result of:
- The dentist missing a canal during the initial treatment
- A canal being incompletely treated (i.e. the tip of the canal left untreated)
- Tissue left inside the tooth
- A fracture to the root
- Leakage of bacteria
If any of these complications arise, your dentist or endodontist will assess your tooth to see whether root canal re-treatment can be performed. The procedure steps for this re-treatment are similar to the original treatment, although more complicated to perform.
In most cases, the alternative to root canal re-treatment is extraction. Patients who don’t wish to undergo further root canal therapy may instead choose to have the problem tooth replaced with a dental bridge or implant.
If a root canal fails because of a re-infection at the tip of the root, it may be possible to perform endodontic surgery. This involves making a small incision in the gum to access the root tip directly. This allows the original structure from the previous treatment to remain in place.
If you are concerned you may have root canal failure, contact your dentist as soon as possible. They are trained to recognise the symptoms of a failed root canal. The earlier it is treated, the less opportunity there is for the bacteria to cause more damage.
Conclusion
Root canal treatment is an effective way to repair a damaged tooth and prolong its life for many years, in some cases even a lifetime. Many people worry that the treatment will be painful, but thanks to modern technologies, the procedure is of minimal discomfort and pain.
Root canal treatment costs in the UK can average £250 to £500 per tooth with a private dentist. The NHS root canal cost falls under the Band 2 charge and has a much lower fixed price. The NHS cost varies anywhere between £47.00 and £70.70, depending on your location in the UK.
It’s normal to experience some sensitivity for a day or two after a root filling, and you are allowed general painkillers to help with the recovery process. If you start to feel pain several days or months after treatment, contact your dentist immediately to consider re-treatment or extraction of a failed root canal.
Remember, regular dental checkups are the best way to pick up on any dental problems before they reach your tooth root. Taking good care of your teeth will help minimise the chances of you needing a root canal treatment in the future.
And remember, you can chat with a dentist at any time — 24/7 about your root canal. A team of certified dentists is standing by at JustAnswer.
FAQs
What does root canal treatment cost in the UK?
Root canal prices with a private dentist in the UK range from £100 – £350 for front teeth and £300 – £700 for back teeth. The NHS root canal cost falls under the Band 2 charge and has a much lower fixed price. The NHS cost varies anywhere between £47.00 and £70.70, depending on your location in the UK.
Is root canal treatment painful?
Fortunately, the anaesthetic technology used by dentists means that the procedure can be performed with minimal discomfort. The procedure should feel similar to having a regular filling, except it will take longer and you may feel stiff afterwards since you have held your jaw open so long.
When do I need root canal treatment?
The root canal system is located in the roots of each of your teeth. A tooth root infection, if left untreated, can cause irreparable damage to the tooth and even spread to other parts of the body. Symptoms that indicate that tooth pulp has become infected may include sensitivity to hot/cold or sweets, pain, swelling, pain to biting or pressure, and a bad taste in the mouth.
What are the signs of infection after a root canal?
If you start to experience severe pain or swelling a few days after treatment, this can be a sign of infection. You may also notice that the tooth becoming discoloured. Speak to your dentist if you have any concerns ahead of your scheduled checkup.
National Library of Medicine: Rubber dam use during post placement influences the success of root canal-treated teeth. Consulted 18th March 2021.
Wiley Online Library: Factors influencing the success of conventional root canal therapy—a five‐year retrospective study. Consulted 13th November 2019.
British Dental Journal: Shaping the root canal system. Consulted 16th October 2020.





