Having inflamed dental pulp tissue, a condition known as pulpitis, can make your teeth very painful. Fortunately, it’s not too difficult to treat and reverse pulpitis, especially if it’s caught early. If you have been diagnosed with pulpitis or you’re worried you might have it, this guide will help you understand more about the condition.
Perhaps you’re confused about the different terms you’ve heard? Chronic and acute pulpitis, reversible and irreversible pulpitis… what do they all mean? In this article we’re going to explain:
- The different types of pulpitis
- What causes it
- How it’s diagnosed
- Pulpitis treatment options, including on the NHS
Pulpitis is just one of the problems that can cause dental pain. If your teeth hurt, whatever you think the cause may be, we recommend you go for a dental checkup before it gets any worse. But for now, here’s all you need to know about pulpitis pain and treatment.
What is pulpitis?
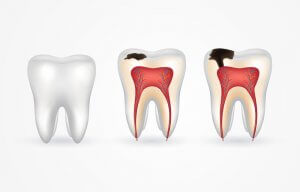
Dental pulpitis is caused by the pulp in your teeth becoming infected or inflamed. Your teeth have three layers: enamel, dentin, and dental pulp. Each layer has a different structural purpose.
- Enamel – the hard outer coating that protects your teeth
- Dentin – the middle layer which supports the enamel
- Dental pulp – the innermost layer with the tooth’s nerves and blood supply
When the inner pulp layer gets exposed or becomes irritated, this can lead to pulpitis. Later on we’ll go through some of the reasons this might happen.
There are two main types of dental pulp inflammation: irreversible and reversible. Irreversible pulpitis means the infection or inflammation has gone so far that the pulp of the tooth can’t be completely saved. In contrast, reversible pulpitis can be treated and fixed if it’s caught early.
Another way that the problem can be categorised is acute pulpitis vs chronic pulpitis. The difference between acute and chronic pulpitis is that with acute pulpitis the pain comes on all of a sudden and can be quite intense, whereas chronic pulpitis is characterised by duller but longer-lasting pain.
Pulpitis symptoms and signs

Most of the time, pain is the first sign of pulpitis in a tooth. This table is a quick guide to the different symptoms you might experience, according to the type of inflammation you have:
Symptom | Reversible Pulpitis | Irreversible pulpitis | Chronic pulpitis | Acute pulpitis |
General pain | Moderate | Intense, throbbing | Low, dull ache | Intense, throbbing |
Teeth sensitivity | Short and sharp | Lasts for more than 30 seconds | Short and sharp | Very painful |
Swelling around teeth | Rarely | Yes | Rarely | Yes |
Fever | Unlikely | Yes | Unlikely | Yes |
Bad breath | No | Yes | Possibly | Possibly |
Increased pain when lying down | No | Yes | No | Yes |
If you experience any of these symptoms you should visit a dentist as soon as possible. Irreversible pulpitis pain can be extreme and sometimes even over-the-counter painkillers won’t help with pulpitis pain relief. If your pulpitis pain becomes unbearable you should seek an appointment with an emergency dentist.
What causes pulp inflammation and infection?
There are quite a few different ways that dental pulp can become inflamed. The most common cause of pulpitis is deep cavities, which expose the pulp to bacteria. Tooth pulpitis occurs when the pulp is irritated or develops an infection.
Some other ways that dental pulp can become inflamed or infected include:
- Injuries or impact around the head or mouth
- A cracked or fractured tooth that exposes the pulp layer
- Severe abfractions (wear) caused by aggressive tooth brushing and/or abrasive toothpaste
- Grinding teeth (bruxism) causing teeth to crack or enamel and dentin to wear away
- A bad bite, or malocclusion, which can cause extra wear on certain teeth
Although uncommon, it is also possible to get tooth pulp inflammation from routine dental visits. For example:
- Pulpitis after a filling can occur because of teeth being exposed to extreme heat when setting the materials.
- The heat caused by tooth polishing may cause inflammation.
- Dental pulp can be exposed to bacteria during a filling treatment.
- Having a crown fitted can irritate the pulp and compromise the nerve.
Getting sensitive teeth after a filling is relatively normal, however, if it lasts longer than a few days you may have pulpitis. If you believe you have dental pulp inflammation because of dental treatment, speak to your dentist to resolve the complaint. You also have the right to make a complaint about your dentist. Here is an NHS guide about how to resolve complaints about your NHS or private dentist.
Diagnosis of pulpitis
Pulpitis diagnosis is fairly straightforward for your dentist. Four types of test can be done to determine if you have this condition and whether it is reversible or irreversible.
- X-rays can show your dentist the extent of the tooth decay and whether it might be possible to reverse the damage.
- Exposure to heat, cold, and sweet things will help your dentist know if the nerve in your tooth is still intact.
- Tooth tap tests are done to tell your dentist how inflamed your tooth is.
- Electric testing involves passing a small electrical current through the tooth. If you can feel the electricity this means your tooth is still alive and the pulpitis is reversible.
The video below explains what pulpitis is and what the differences are between reversible and irreversible pulpitis:
Treatment options
Since there are several types of pulpitis, there are also several treatments. Your dentist will complete some tests to see whether your tooth can still be saved, and offer you pulp inflammation treatment accordingly.
Reversible pulpitis treatment
Your tooth can be saved if you seek early treatment for reversible pulpitis. Your dentist will remove any cavities and add a filling to stop the pulp being exposed. We have a complete guide to teeth fillings which explains more about this process and your different options for tooth fillings. Similarly, tooth pulpitis caused by a crack in the tooth can also be treated, usually with a crown.
Irreversible pulpitis treatment
When the pulp in a tooth has died, it can’t be restored or recovered. However, it may still be possible to save the tooth. With a diagnosis of irreversible pulpitis, dentists can perform a root canal procedure to remove the pulp tissue. The tooth is then filled and sealed, usually with a crown, and should look and feel normal again.
Where root canal treatment isn’t viable, usually because the damage has spread too far, the only remaining pulpitis treatment option is an extraction. After this, there are a number of ways to replace the missing tooth including dentures, a bridge or an implant.
Pulpitis and antibiotics
Some dentists may prescribe antibiotics to try and relieve pain and reduce inflammation in cases of irreversible pulpitis. There isn’t much evidence that antibiotics help in relieving the pain, so if you’re concerned about taking antibiotics for pulpitis chat with your dentist.
If left untreated, pulpitis can lead to a dental abscess, which is a pocket of infection at the base of the tooth around the gums. In this case, antibiotics are likely to be used as part of a larger course of treatment to remove the infection and treat or extract the tooth causing the problems.
Frequently asked questions
How can I prevent pulpitis?
Pulpitis is pretty easy to avoid. Since the most common cause of pulp inflammation is cavities and decay, you can avoid foods with lots of sugar and acid to protect your tooth enamel. Having a good oral hygiene routine will certainly help too; brushing, flossing, and using mouthwash regularly all work towards preventing decay.
Also, be sure to have regular checkups and dental cleanings at the dentist. A cavity spotted early can be filled before it gets anywhere near the pulp to cause painful problems.
How long does reversible pulpitis last?
As soon as you have the cavity removed, your pain and inflammation should stop. It’s really important to get to a dentist as soon as possible when you get any type of toothache. Catching pulpitis early can mean the difference between a simple filling and a lengthy root canal treatment, or even losing the tooth entirely.
Can I get treatment for pulpitis on the NHS?
As is standard, any non-cosmetic dental treatment will be free for children under the age of 18. For adults, pulpitis treatment will normally fall into band 2 which costs £65.20. This covers fillings, root canals, and extractions. Our guide to NHS dental costs contains more information.
If you’ve had to have a tooth extracted and want to replace it, you should be able to get a denture or a bridge on the NHS, while implants will need to be paid for privately.
Conclusion
There are two main types of pulpitis: reversible and irreversible. Both occur when the innermost layer of the teeth, the pulp which holds the nerves and blood supply, gets inflamed. Pulpitis pain can be intense in the case of acute pulpitis, or weaker in the case of chronic pulpitis.
Treated early, reversible pulpitis can be fixed with a simple filling. Without early intervention, the pulp can die and the problem becomes irreversible. At this point, the only options are root canal treatment or tooth extraction.
Oral health problems like this are generally avoidable with good oral hygiene and regular dentist visits. It’s not a nice problem to encounter with your teeth, so prevention is definitely better than a cure.
CDA Oasis: What is the best antibiotic to prescribe for irreversible pulpitis? Consulted 24th August 2019.
MSD Manual: Pulpitis. Consulted 24th August 2019.
NHS: How do I complain about my dental treatment? Consulted 24th August 2019.




