Are you worried you might have a tooth abscess? Or maybe your child does and you’re wondering how to treat an abscessed tooth. A mouth abscess is a serious medical issue that needs to be addressed promptly. And you’ll want to resolve it quickly because tooth abscess pain can be quite severe.
Thankfully, your dentist will be able to help you with swift abscessed tooth treatment, including tooth abscess antibiotics if the mouth infection is severe.
If you feel like you might need urgent care or pain relief, did you know you can connect with a dentist in your state right now for an online consultation? This is a service provided by Denteractive. Opt for a video call and the dentist will be able to prescribe you pain medication and antibiotics, if needed. Click here to read full details and get started.
To help you on your quest to learn more about oral abscesses, in this article we’ll answer the following questions:
- What is an abscessed tooth?
- What causes dental abscesses?
- Which tooth abscess symptoms should I look out for?
- What does abscessed tooth treatment involve?
- What are the best antibiotics for an abscessed tooth?
- How do you know if a tooth infection has spread?
We also have some tips for avoiding oral infections and keeping your mouth in a healthy state.
Before we dive in, if you need to speak to a dentist right now about an infection, and you can’t get in to see one, you can consult with a dentist, online right now:
What is an abscessed tooth?
A tooth abscess, or a dental abscess, is a pocket of pus that accumulates when a bacterial infection breaks down tissue. Normally this mouth abscess visibly manifests as an abscess on the gum. Abscesses can form in many different parts of the body. They are a natural defense mechanism, the aim being to block the infection from reaching other areas. The resulting build-up of pus is usually very painful.
When it comes to mouth abscesses, both the gums and the teeth themselves are at risk. A dental abscess in the mouth can erode the periodontal structure (which supports the teeth) and the jaw bone, causing irreparable damage. In some cases, you may need a tooth extraction.
By understanding tooth abscess symptoms and seeking professional tooth infection treatment as soon as you become concerned, you can reduce the chances of further infection and complications.
Types of dental abscess
There are three main types of oral abscess: gingival, periodontal, and periapical. The distinguishing factor for each one is the location where the abscess forms.
Gingival abscess
A gingival abscess, or gum abscess, is an abscess in the gum that forms on the surface of the tissue at the gum line of the teeth (gingiva). For some people, a gum abscess looks somewhat like a pimple on the gum. This mouth abscess on the gum is often a result of external damage to the gum, for example from food entering the gumline. You may also experience an abscessed gum from damage like penetration from a toothpick.
If caught early, a mouth abscess on the gum is relatively easy to treat and recover from. If left untreated, however, abscessed gums can progress to a periodontal abscess and cause greater oral damage.
Periodontal abscess
Unlike an abscessed gum, this type of tooth abscess occurs deeper into the gum pockets. Since there is nowhere for pus to drain, the mouth abscess spreads into the surrounding tissue and jaw bone.

Periapical abscess
This type of mouth abscess begins in the soft tooth pulp, usually as a result of decay deep inside the tooth. Once tooth decay has eroded the protective enamel and dentin of the tooth, bacteria can invade the nerves and tooth pulp.
Pus from this infection may appear at the gum line of the tooth, similar to an abscessed gum, but more commonly it ends up in surrounding tissue which becomes inflamed.
Wisdom tooth abscess
Wisdom tooth abscesses are a particularly common type of periapical abscess, since the very back teeth are harder to clean. In addition, it’s harder for your dentist to spot cavities on these teeth and treat them early on.
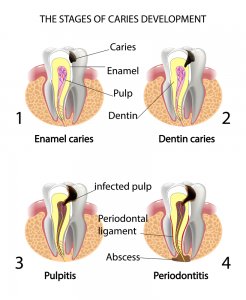
Tooth abscess stages
The different tooth abscess stages can be summed up into three parts:
Tooth decay: This is the first stage of an abscessed tooth. The build-up of bacteria on the surface of the tooth create plaque. The plaque eats away at the tooth enamel and a cavity is formed. The bacteria works its way through the tooth and into the dentin layer. Once the bacteria get through the dentin and enter the pulp, you’ve got the beginning of your tooth abscess.
Infected pulp: The second of the tooth abscess stages is infection of the pulp (pulpitis). The bacteria is now in the tooth pulp, causing the pulp to become infected. Nerves begin to die, the immune system goes after the infection and more inflammation results. Pus is formed around the dying tooth root, causing the dental abscess.
Spreading of mouth infection: If the tooth abscess makes it to the third stage, it can begin to spread the infection to other parts of your mouth. The tooth abscess may chip away at bone tissue, and it can spread along the jaw bone. If never treated, it can even be fatal.


Causes of abscesses in the mouth
Your mouth naturally contains bacteria, and when not cleaned well, this bacteria forms plaque on your teeth and gums. Teeth infections develop when the acid produced by plaque starts to decay the teeth or gums.
As mentioned above, abscesses most commonly occur when tooth decay is left to spread. Other possible reasons for infection include:
- Gum disease (gingivitis)
- A cracked tooth
- Trauma
- Complications from dental surgery such as implants, root canal treatment, and extractions
- Rough tooth brushing
- Food stuck between teeth and gums
People with poor dental hygiene are more susceptible to oral abscesses due to an increased build-up of plaque. Any injury or surgery to teeth and gums can increase the chances of infection as delicate parts of the mouth are exposed to bacteria.
In addition, people with a weakened immune system are at greater risk of developing a dental infection leading to a mouth abscess. The immune system is affected by certain underlying health conditions, such as diabetes. Some medical treatments, such as chemotherapy, also reduce a patient’s natural immunity.
While none of these things will automatically lead to a tooth or gum abscess, they are all factors that increase the risk of mouth infection.
Tooth abscess symptoms
In most cases, symptoms of an infected tooth are not demure. Instead, your abscessed tooth symptoms are likely to include strong pain and difficulty eating. Specifically, dental abscess symptoms include:


- Continuous, throbbing pain
- Pain when the tooth is tapped
- Increased pain when eating hot or cold foods/drinks
- Greater discomfort when biting teeth together or chewing food
- A foul, bitter taste in the mouth from draining pus
- A bad smell in the mouth from the infection
- Swelling and reddening of the face or gums
- Bleeding gums
- A tooth that is loose and/or discolored
- A pea-sized bump on gums or pimple inside the mouth
More serious abscessed tooth symptoms which may indicate dental abscess complications include:
- Fever
- Headache
- Nausea
- Diarrhea
- Swollen lymph glands
- Pain spreading to the jaw, ear or neck on the same side as the infected tooth
- Difficulty opening your mouth (trismus)
- Difficulty breathing or swallowing (dysphagia)
- General fatigue
These symptoms of an infected tooth usually come on quite suddenly. Within a few hours, you may find yourself in excruciating pain.
Note that patients can experience an initial toothache as part of their abscessed tooth symptoms, which then fades away. It’s easy to assume that the problem is fixed, but this is not the case. Your tooth pulp cannot heal itself, but once the nerve is destroyed you won’t experience any pain. It’s only once the infection has spread through the dead tooth into the surrounding gums and tissue that the tooth abscess symptoms will re-appear. At this point, far more extensive damage has been done.
To avoid tooth abscess complications, you should visit a dentist as soon as you notice any tooth infection symptoms, even if they disappear by themselves.
If you’re not sure what your symptoms mean, you can talk to a dentist right now with Denteractive. They have a network of dentists across the USA available for free text chat or a video consult. They’ll be able to assess your tooth abscess symptoms and advise you on the best course of action, even prescribing antibiotics if appropriate.
An online video consultation can also be a good option if you’re in severe pain or worried about infection but can’t get to a dentist right now.
Acute oral abscess vs. chronic oral abscess

The above dental abscess symptoms are all characteristic of what is called an acute dental abscess. This spreads fast and usually causes great discomfort and pain for the patient.
A chronic dental abscess, on the other hand, grows slowly and may cause no pain whatsoever. The patient is therefore unaware of the presence of the abscess, and only a dental x-ray will be able to identify it. This is usually a periapical abscess, spreading gradually through the tooth root and into the surrounding tissue.
Eventually, the pus may create a tunnel through the bone and tissue, known as a ‘fistula’ or ‘sinus tract’. This allows the pus to drain, and looks like a pimple inside your mouth. If you see or feel something like this in your mouth, even if you haven’t experienced any other tooth abscess symptoms, you should consult your dentist. If pus starts to drain through the fistula, you’ll know about it from the foul taste.
What does an abscessed tooth look like?
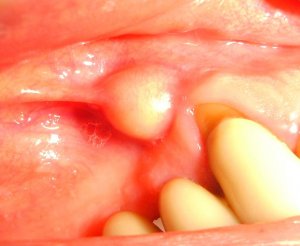
If you think you may have a dental abscess, you might be searching for abscessed tooth pictures to find out what an abscess in the mouth looks like. Keep in mind that not all abscesses are externally visible, so don’t put off visiting your dentist just because you can’t see any outward signs of infection.
While some mouth abscesses may appear as a small lump inside the mouth (as in the image above), some symptoms of an infected tooth manifest in much greater swelling either in the mouth or on the face.
Abscessed tooth pictures
These abscessed tooth pictures show some different aspects of what a mouth abscess looks like:
Yes, some of these tooth abscess pictures are quite alarming, but if you recognize these dental abscess symptoms, take a deep breath, stay calm and contact your dentist, who will skillfully help you through the treatment process. Make sure you get professional care ASAP, to avoid becoming one of the thousands of people who are hospitalized for dental abscesses each year.
Tooth abscess treatment
Dental abscess pain can be intense and prevent the patient from eating properly. In this case, it may be appropriate to seek emergency dental treatment. Even if the tooth abscess pain is bearable, you should visit a dentist as soon as possible to avoid further damage and complications. You can call 866-383-0748 to find a dentist available near you, 24/7.
If you’re having difficulty breathing or swallowing, or have a fever or facial swelling, call 911 or get straight to an emergency room. These are symptoms of the tooth infection spreading further into your jaw and possibly bloodstream, so you need urgent tooth abscess treatment.
You may be wondering how to get rid of a tooth abscess without going to the dentist. Well, simply put, there’s no safe way. Because abscesses are caused by harmful bacteria, treatment can be very dangerous without the proper tools and training.
For a professional, gum abscess treatment is relatively straightforward. Your dentist may begin by taking an x-ray to determine how far the abscess has spread and what kind of treatment is needed. Then, the first priority with any dental abscess treatment is to drain the pus that has built up and remove the source of the infection.
Draining a gum abscess
The method for doing this will depend on the type of mouth abscess. It may be possible to release the pus by applying gentle pressure, just as you would with a pimple on your skin. (Don’t try this treatment at home, your dentist will know how to drain a gum abscess safely and effectively.) The dentist will then use a small probe to scrape the remaining infected material from inside the abscess.


In other cases, the dentist may have to make a small incision in the gum tissue to access the infected area.
Provided the infection hasn’t spread into the periodontal structure, no further tooth abscess treatment will be required although antibiotics for tooth infection may aid recovery.
If you have a gum abscess which ruptures by itself, you may find that the pain subsides significantly when the pressure is released. However, this doesn’t mean the mouth infection has cleared. You should still visit your dentist to have the area cleaned properly.
Where a fistula has formed on the gum because of a periodontal abscess, the dentist will insert a thin probe into the hole. They will then take an x-ray (with the probe still in place), and from this, they can see the original source of the infection.
Again, if you’re wondering how to drain a tooth abscess at home, you shouldn’t. A dentist is the best person to carry out this procedure.
If you are unsure how urgently you need treatment for your tooth abscess, chat online with a licensed US dentist within minutes with Denteractive. Dentists are available for a live video call or text chat 24/7, every day of the year.
Root canal treatment for abscessed teeth
Periapical abscesses can often be treated with a root canal. This involves drilling down through the crown of the tooth to access the infected pulp chamber. The dentist drains the pus from the abscess, cleans and disinfects the cavity, and applies a filling material. If the tooth has been weakened, a dental crown can help prolong its life.
Find more information on root canal procedures here, or watch this short video explaining how root canal treatment is conducted:
Tooth abscess complications
If your abscess goes untreated, there are some serious abscess complications that could lead to extraction. In the case of periapical and periodontal abscess treatment, if the infection has spread into the jaw bone or periodontal ligament it may be necessary to extract one or more teeth. Extraction is a last resort, though, and will only be done if the dentist judges the bone to be too far eroded to support the teeth.
With periodontal abscess treatment, the dentist will first carry out a deep cleaning of the gum pocket. He or she can then assess the extent of the infection. Oral x-rays will also reveal how far the infection has spread.
The abscess may have caused the tooth to become loose, and in this case, an extraction may be the only solution. Extraction may also be necessary in cases where re-infection occurs after abscess removal, or when infection occurs in a tooth that has already undergone root canal treatment.
Medication for dental abscess treatment
After abscessed tooth treatment, any remaining pain can be managed with common over the counter painkillers like Ibuprofen and Tylenol. Unless prescribed otherwise, adults may take 200-400mg of ibuprofen every 6-8 hours, up to a maximum of 1200mg every 24 hours. For acetaminophen (Tylenol/paracetamol) the recommended dose is 325-1000mg every 4-6 hours, up to a maximum of 4000mg (eight 500mg tablets) in 24 hours.
Along with OTC painkillers, your dentist will recommend plenty of rest and limiting your chewing to soft foods only until you are fully recovered.
Treatment with tooth abscess antibiotics
If you think you have an abscess, you’ll be wondering how to treat an abscessed tooth. Depending on the severity of the abscess, the dentist may prescribe an antibiotic for the tooth infection. Dental abscess antibiotics are usually only issued when the patient has a fever or the infection is particularly widespread. Some of the most common tooth abscess antibiotics include:
- Penicillin: Penicillin is one of the most common antibiotics for an infected tooth.
- Amoxicillin: Amoxicillin is in the same class as penicillin and is another of the common antibiotics for an abscessed tooth. Read more about how long amoxicillin takes to work on a toothache.
- Metronidazole: Your dentist may prescribe you metronidazole along with penicillin to cover various kinds of species of bacteria.
- Clindamycin: This may be the best antibiotic for your tooth infection if you are allergic to penicillin.
- Erythromycin: This is another example of antibiotics for an abscessed tooth that you may be prescribed if you have allergies to the more common antibiotics like penicillin.
If your dentist does prescribe antibiotics for a gum abscess, they will tell you about the dosage and how long your tooth abscess antibiotics will take to work. You should mention if you have any sensitivity or resistance to specific antibiotics.
It’s important that you follow your dentist’s instructions for taking antibiotics for a mouth infection. Always finish the full course of treatment, even if you feel better before the medicine is finished. If you still feel unwell after completing your antibiotic treatment, call your dentist.
If you miss a dose, take it as soon as you remember, unless it is almost time for your next dose. In that case, skip the missed dose and continue your prescribed schedule. Don’t double dose to make up for a missed one.
Take the capsules with a full glass of water so that the medication will not irritate your throat.
-Renad S. Nahhas, Pharmacist
How much does it cost to treat an abscess in the mouth?
There is no fixed cost for mouth abscess treatment. Not only do charges for tooth infection treatment vary from one dentist to another and between regions, but the type of treatment required for a dental infection will differ for each patient. Many dental insurance policies will reimburse some or all of the costs incurred for tooth infection treatment. Read more about the best dental insurance policies.
What to ask your dentist about an abscessed tooth
If you suspect you have a mouth abscess, here are some questions you may wish to ask your dentist at your appointment:

- What are the symptoms of a tooth infection?
- Which type of oral abscess do I have?
- What tooth abscess treatment do you recommend?
- Are there any other options for tooth infection treatment?
- How long will tooth abscess treatment take, and how many visits will I need?
- Will I need to take time off work to recover?
- How often should I come for check-ups in the future?
- What oral care products do you recommend?
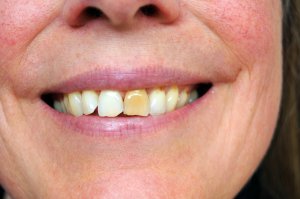
In some cases, damaged teeth become discolored over time. You may want to ask your dentist how likely this is in your case, and what tooth whitening options may be available if you do experience tooth discoloration.
How to treat a tooth abscess at home
If you have a painful abscessed tooth and a swollen face, you will probably be looking for an immediate home remedy. Although the only way to be sure of effective treatment for an abscess in the mouth is with a visit to the dentist, there are some tooth and gum abscess home treatments which can help alleviate the pain and stop the infection from spreading further while you wait for your appointment.
The best form of tooth abscess pain relief is ibuprofen, but acetaminophen (Tylenol) is second best. If you find just one of these ineffective, you may take both ibuprofen and acetaminophen up to the maximum doses shown on the packets.
Other ways to relieve tooth infection pain include:
- Rinsing and gargling with warm salt water
- Avoiding hot or cold food and drink
- Eating only soft foods
- Avoiding flossing around the affected area
- Using a soft toothbrush
Read more about ways to relieve tooth infection pain at home.
Antibiotics for tooth infection pain must be prescribed by a dentist. If you don’t seek professional tooth abscess treatment, it is likely the infection will keep spreading. This can lead to serious damage to your teeth, periodontal ligament, and jaw bone. The infection might spread to other parts of your body if left long enough.
If you can’t get an appointment to see your usual dentist right away, we recommend you get a live online consultation using Denteractive. Choose the video call option and, following an assessment, the dentist should be able to prescribe you stronger pain medication and antibiotics. This should provide some immediate relief from your tooth abscess pain while you wait for treatment in-person.
Alternatively, use their free dentist chat option to just receive medical advice about your situation.


Remember that just because an abscess has drained and the pain has subsided, this doesn’t mean the infection is gone. You still need to visit a dentist for tooth abscess treatment.
How to prevent tooth and gum abscesses
Maintaining good oral health will minimize your chances of developing a gum abscess or a tooth abscess. There are many steps you can take to keep your teeth and gums as healthy as possible:

- Brush twice a day with fluoride toothpaste and floss or use an interdental brush at least once a day
- Avoid consuming sugary drinks and foods as snacks between meals or just before going to bed
- Where possible, brush soon after consuming foods and drinks with a high sugar or starch content
- Regularly visit your dentist to have oral check-ups
Even if you do develop dental cavities because of tooth decay, the affected tooth or teeth can be treated with a filling before the tooth pulp becomes infected and results in an abscessed tooth. This is far preferable to undergoing root canal treatment or an extraction for an abscessed tooth, so regular trips to the dentist are very important.
How to prevent a wisdom tooth infection
If you still have your wisdom teeth, especially if they haven’t emerged properly, speak to your dentist about your concerns about having an abscessed tooth, and whether it would be wise to have them removed. Since wisdom tooth abscesses are relatively common, having the teeth removed is often the best way to prevent infections, an abscessed tooth, and other complications.
Finally, you should seek dental care if you experience any trauma to your teeth, for example chipping or cracking. Even if there is no immediate pain, bacteria can invade the tooth immediately and a dental infection like an abscessed tooth may develop within days.
Conclusion
Now you know more about what a tooth abscess is, some symptoms to look for, and how to know if a mouth infection has spread. You also know a bit about abscessed tooth treatment options, and the importance of seeing a dentist so they can clean the infected tissue and prescribe antibiotics if needed.
So, if you notice a painful pimple on your gum, pus pockets on your gums or any other tooth infection symptoms, you should make sure to see your dentist. An abscessed tooth is serious, and often stems from a problem like tooth decay. Additionally, if your tooth abscess pain is so severe that you can’t eat, you should consider it a dental emergency.
Call 866-383-0748 to connect with a dentist open now near you, to get the treatment you need right away.
Alternatively, you can use Denteractive’s online consultation service to speak to a dentist 24/7 about your problem. They have a network of dentists licensed in each state ready to assess your situation and prescribe medication, if needed. You can also find out more about this online dental service in our teledentistry guide.
FAQs
How do you drain a tooth abscess at home?
One of the abscessed tooth symptoms is a pus pocket on the gums, it might look sort of like a pimple on your gum. As part of your dental abscess treatment, your dentist will drain the abscess. Although the treatment might seem relatively straightforward, you should not try to drain your abscess at home! Only a dentist will know how to drain a gum abscess in a safe and effective manner.
Will a tooth abscess go away with antibiotics?
Although a tooth abscess may need additional treatment, your dentist might prescribe an antibiotic for your infected tooth. Some common tooth abscess antibiotics include penicillin and amoxicillin. Your dentist will be able to determine what exactly is needed to treat the abscess in your jaw.
What does a gum abscess look like?
Visible symptoms of abscessed gums can include pus pockets on the gum and swelling in your mouth or on your face. It may also manifest as a bump that looks like a pimple on the gum.
Can I have a gum abscess with no pain?
Although one of the most noticeable abscessed tooth symptoms is pain, an abscessed gum can sometimes cause little to no pain. Even if you aren’t experiencing pain, you must seek treatment. A mouth abscess won’t cure itself.
What are the symptoms of a tooth infection spreading to the body?
In addition to localized pain, signs of a tooth infection spreading include feeling generally unwell, headache, fever, swelling, increased heart rate, dehydration and stomach pain. If your abscessed tooth symptoms have taken a turn for the worse, you need to seek emergency medical attention.
What are the best antibiotics for an infected tooth?
The best antibiotic for a tooth infection will be the one prescribed to you by your dentist. That being said, tooth abscess antibiotics include penicillin, amoxicillin, clindamycin, and erythromycin.
Are there any over-the-counter antibiotics for an infected tooth?
No, there are no over-the-counter antibiotics, nor home remedies for a tooth abscess. Your dentist will prescribe you antibiotics for your infected tooth if necessary. After making an appointment to see your dentist for your abscessed tooth treatment, you can take painkillers like ibuprofen or Tylenol to ease the tooth abscess pain.
If you can’t get to a dental clinic for some reason, you can have an online consultation to receive the prescription you need.
How long does it take for amoxicillin to work with a tooth infection?
How long it takes antibiotics like amoxicillin to work varies by patient, though symptoms usually subside after only a few doses. That said, it is very important to finish the entire course of antibiotics. Finishing the whole course (usually 3-10 days) will avoid the infection returning stronger than before. It’s not easy to tell how an abscess is healing once the symptoms subside, but if they come back you know that it did not heal.
Can you get rid of a tooth infection without antibiotics?
In the case of a serious tooth infection, your dentist may tell you that you need to take antibiotics in order to cure it. If that is the case then it is important to do as your dentist says. There are cases, however, if your infection isn’t severe, where your dentist may simply drain the pus pocket on your gums, and have no need to prescribe you antibiotics for a tooth infection.
Nytimes.com: Oral Infections Causing More Hospitalizations. Consulted 12 September 2019.
NCBI: Dental Abscess. Consulted 12 September 2019.








